Copyright © 2014: Manila Retina Specialists All Rights Reserved
Diabetes can adversely affect the eye, depending on the duration of disease. Diabetes may cause narrowing of the blood vessels, which may cause ischemia, or lack of blood supply to the eye. This causes development of new vessels, which can bleed, or easily leak, causing macular edema.
 Fig 13a Proliferative Diabetic Retinopathy Fig 13a Proliferative Diabetic Retinopathy | 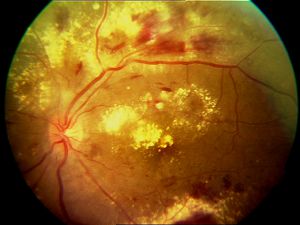 Fig 13b Diabetic Macular Edema Fig 13b Diabetic Macular Edema |
If caught early, your doctor may recommend Panretinal Photocoagulation (PRP), which is laser treatment to the periphery of the retina. This reduces the chance of bleeding by almost 50-90%. Side effects include narrowing of your field of vision, and/ or delay in adapting to dark conditions. Most of diabetic retinopathy is asymptomatic, so we recommend at least a yearly exam if you are diabetic. Sometimes there is sudden onset of blurred vision, which may be due to bleeding in the gel of the eye (vitreous). This is called vitreous hemorrhage.
Sometimes, membranes may form on the surface of the retina, causing traction retinal detachment. If it involves the central vision (macula), your doctor may recommend surgery to remove the membranes.More often, there is gradual, almost imperceptible loss of central vision, and you notice difficulty reading small print. This is caused by accumulation of fat deposits in the macula, called clinically significant macular edema. this is a leading cause of visual loss in diabetics.
If you have macular edema, your doctor will get OCT (optical coherence tomography) studies to determine the extent of swelling. This will serve as a guide to treatment. Anti-VEGF therapy may be recommended alone, or combined with focal laser. Steroid implants (Ozurdex) has also recently been approved for this condition as well.
TYPES OF DIABETIC RETINOPATHY
- Non- Proliferative ( Background) Diabetic Retinopathy- retinal blood vessels can develop leaks and retina becomes wet and swollen. Fat can accumulate in the macula (part of the eye which is used for reading), and cause permanent damage. This is known as clinically significant macular edema.
- TREATMENT-
- Anti-VEGF (vascular endothelial growth factor) injection is done to stop abnormal retinal blood vessels from leaking and to dry up the fat deposits. Vision improvement depends on duration of the macular edema, and pre injection vision. A loading dose is usually given, after which maintenance dose will depend on the response. We use Avastin (not FDA approved), or Lucentis, Eylea, Vabysmo.
- Steroid Implant (Ozurdex)- This is now US FDA approved for diabetic macular edema. The main advantage is that it can be given less frequently , eg every 3-6 months, due to its longer half life. After injection, we need to monitor the intraocular pressure (iop).
- Focal Laser or Subliminal Threshold Laser- This was preferred treatment before, but now is used only if unresponsive to anti-VEGF. It does not usually improve vision, but can minimize further loss of vision. In some patients, all the leaking spots may be properly treated, but they may continue to leak, or new ones, may develop. In such cases, further leakage causes more swelling and worsening of vision.
- TREATMENT-
- Proliferative Diabetic Retinopathy - cause by closure of the blood vessels in which neovascularization (growth of abnormal new blood vessels) develops. This may lead to the following complications:
- Vitreous Hemorrhage - bleeding in the vitreous cavity. Patient may notice sudden appearance of floaters, spider webs, spots in front of the eye, or blurred vision
- Traction Retinal Detachment - neovascularization develops and this leads to growth of scar tissue on the retina. the scar tissue can pull the retina off the back wall of the eye. The patient may notice a shadow or large dark area in his vision. Scar tissue can cause visual loss because it can wrinkle the retina.
- Rubeosis -when ischemia or non perfusion is severe, neovascularization grows in the iris. It may close off the normal flow of fluid out of the eye and can cause increase pressure in the eye (called Neovascular Glaucoma)
- TREATMENT
- Pan retinal Photocoagulation laser can be used to destroy all the dead areas of the retina. When these areas are treated with the laser, the retina stops manufacturing new blood vessels, and those that are already present tend to decrease or disappear.
- Anti-VEGF (neovascularization) injections In some cases of vitreous hemorrhage, injections alone may allow bleeding to absorb. It has also been shown to be as good as laser treatment, but this option entails frequent injections and follow up.
- Pars Plana Vitrectomy If laser is not possible and the blood does not disappear on its own, it can be remove with an operation called Pars Plana Vitrectomy. This surgery is done in the hospital or ambulatory surgical center, under general or local anesthesia. This procedure also used to remove the blood and scar tissue. Surgeon may also do laser intraoperatively, to prevent later development of neovascularization and to seal any tears in the retina. If there are tears, the surgeon may place special gas bubble, or silicone oil inside the eye to press the retina completely against the back wall of the eye while the laser takes hold. The patient should position his/her head facing down for 1-2 weeks after the surgery if gas is used. No air or high altitude (mountainous area) travel for 1-6 weeks, depending on gas used. In time gas bubble will disappear and replace by the eye’s own fluid.
 Fig 14 Dr. Uy and his surgical team doing a Pars Plana Vitrectomy with the Bausch and Lomb Stellaris PC and Zeiss Operating Microscope.
Fig 14 Dr. Uy and his surgical team doing a Pars Plana Vitrectomy with the Bausch and Lomb Stellaris PC and Zeiss Operating Microscope.
